Like what you see?
Sign up to receive more free parenting advice.
Thank you for subscribing to our newsletter!
Child Development
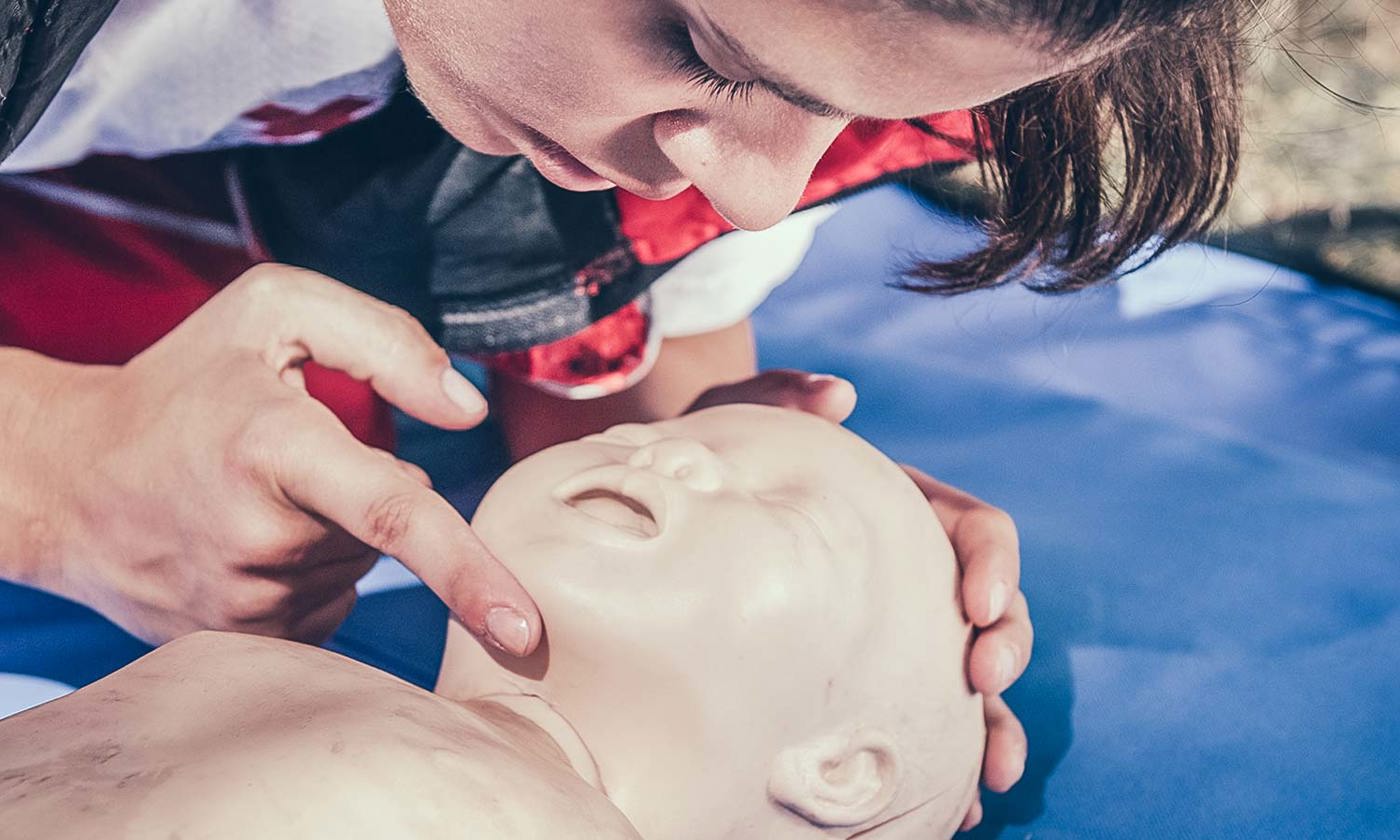
Credit: iStock.com/microgen
In a perfect world every new parent would attend a first aid course to ensure they can resuscitate a child.
If you can’t sign-up for a class right now, take a few minutes to read this detailed cardiopulmonary resuscitation (CPR) sequence for infants (babies under a year old) and children.1 It is however recommended that every parent goes on a first aid course and regularly attend refresher courses so that they understand the processes and remember them.
Of course, in a life-threatening emergency, dial 000. If your child is coughing or wheezy see your GP for advice. For training courses see St John First Aid Training.
Child and baby CPR steps
Ensure the area is safe
- Check for hazards, such as electrical equipment or traffic.
Check your child's responsiveness
- Gently stimulate your child and ask loudly, "Are you all right?".
If your child responds by answering or moving
- Leave them in the position they were found in (provided they're not in danger).
- Check their condition and get help if needed.
- Reassess the situation regularly.
If your child doesn't respond
- Shout for help.
- Carefully turn the child on their back.
If the child is under one year old:
- Ensure the head is in a neutral position, with the head and neck in line and not tilted.
- At the same time, with your fingertips under the point of your child's chin, lift the chin. Don't push on the soft tissues under the chin as this may block the airway.
If the child is over one year old:
- Open your child's airway by tilting the head and lifting the chin.
- To do this, place your hand on their forehead and gently tilt their head back.
- At the same time, with your fingertips under the point of your child's chin, lift the chin. Don't push on the soft tissues under the chin as this may block the airway.
If you think there may have been an injury to the neck, tilt the head carefully, a small amount at a time, until the airway is open. Opening the airway takes priority over a possible neck injury.
Check their breathing
Keeping the airway open, look, listen and feel for normal breathing by putting your face close to your child's face and looking along their chest.
- Look for chest movements.
- Listen at the child's nose and mouth for breathing sounds.
- Feel for air movement on your cheek.
Look, listen and feel for no more than 10 seconds before deciding that they're not breathing. Gasping breaths should not be considered to be normal breathing.
If your child is breathing normally
- Turn them on their side.
- Check for continued breathing.
- Send or go for help – do not leave your child unless absolutely necessary.
If your child isn't breathing or is breathing infrequently and irregularly
- Carefully remove any obvious obstruction in the mouth.
- Give five initial rescue breaths (mouth-to-mouth resuscitation) – see below.
- While doing this, note any gag or cough response – this is a sign of life.
Rescue breaths for a baby under one year
- Ensure the head is in a neutral position and lift the chin.
- Take a breath, then cover your baby's mouth and nose with your mouth, making sure it's sealed. If you can't cover both the mouth and nose at the same time, just seal one with your mouth. If you choose the nose, close the lips to stop air escaping.
- Blow a breath steadily into the baby's mouth and nose over one second. It should be sufficient to make the chest visibly rise.
- Keeping their head tilted and chin lifted, take your mouth away and watch for the chest to fall as air comes out.
- Take another breath and repeat this sequence four more times.
Rescue breaths for a child over one year
- Tilt the head and lift the chin.
- Close the soft part of their nose using the index finger and thumb of the hand that's on their forehead.
- Open their mouth a little, but keep the chin pointing upwards.
- Take a breath, then place your lips around their mouth, making sure it's sealed.
- Blow a breath steadily into their mouth over about one second, watching for the chest to rise.
- Keeping their head tilted and chin lifted, take your mouth away and watch for the chest to fall as air comes out.
- Take another breath and repeat this sequence four more times. Check that your child's chest rises and falls in the same way as if they were breathing normally.
Obstructed airway
If you have difficulty achieving effective breathing in your child, the airway may be obstructed.
- Open the child's mouth and remove any visible obstruction. Don't poke your fingers or any object blindly into the mouth.
- Ensure there's adequate head tilt and chin lift, but the neck isn't overextended.
- Make up to five attempts to achieve effective breaths (enough to make the chest visibly rise). If this is still unsuccessful, move on to chest compressions combined with rescue breaths.
Assess the circulation (signs of life)
Look for signs of life. These include any movement, coughing, or normal breathing – not abnormal gasps or infrequent, irregular breaths.
Signs of life present
If there are definite signs of life:
- Continue rescue breathing until your child begins to breathe normally for themselves.
- Turn the child on their side into the recovery position and send for help.
- Continue to check for normal breathing and provide further rescue breaths if necessary.
No signs of life present
If there are no signs of life:
- Start chest compressions immediately.
- Combine chest compressions with rescue breaths, providing two breaths after every 30 compressions.
Chest compressions: general guidance
- To avoid compressing the stomach, find the point where the lowest ribs join in the middle, and then one finger's width above that. Compress the breastbone.
- Push down 4cm (for a baby or infant) or 5cm (a child), which is approximately one-third of the chest diameter.
- Release the pressure, then rapidly repeat at a rate of about 100-120 compressions a minute.
- After 30 compressions, tilt the head, lift the chin, and give two effective breaths.
- Continue compressions and breaths in a ratio of two breaths for every 30 compressions.
Although the rate of compressions will be 100-120 a minute, the actual number delivered will be fewer because of the pauses to give breaths.
The best method for compression varies slightly between infants and children.
Chest compression in babies less than one year
- Do the compressions on the breastbone with the tips of two fingers, not the whole hand or with two hands.
- The quality (depth) of chest compressions is very important. If the depth of 4cm cannot be achieved with the tips of two fingers, use the heel of one hand – see advice for children, below.
Chest compression in children over one year
- Place the heel of one hand over the lower third of the breastbone, as described above.
- Lift the fingers to ensure pressure is not applied over the ribs.
- Position yourself vertically above the chest and, with your arm straight, compress the breastbone so you push it down 5cm, which is approximately one-third of the chest diameter. The quality (depth) of chest compressions is very important.
- In larger children or if you're small, this may be done more easily by using both hands with the fingers interlocked, avoiding pressure on the ribs.
If nobody responded to your shout for help at the beginning and you're alone, continue resuscitation for about one minute before trying to get help – for example, by dialling 000 on a mobile phone.
Continue resuscitation until
- Your child shows signs of life – normal breathing, coughing, movement of arms or legs.
- Further qualified help arrives.
- You become exhausted.
1 Contains public sector information licensed under the Open Government Licence v3.0.
CPR training
When was the last time you completed or refreshed your CPR training?



