Like what you see?
Sign up to receive more free parenting advice.
Thank you for subscribing to our newsletter!
Child Development
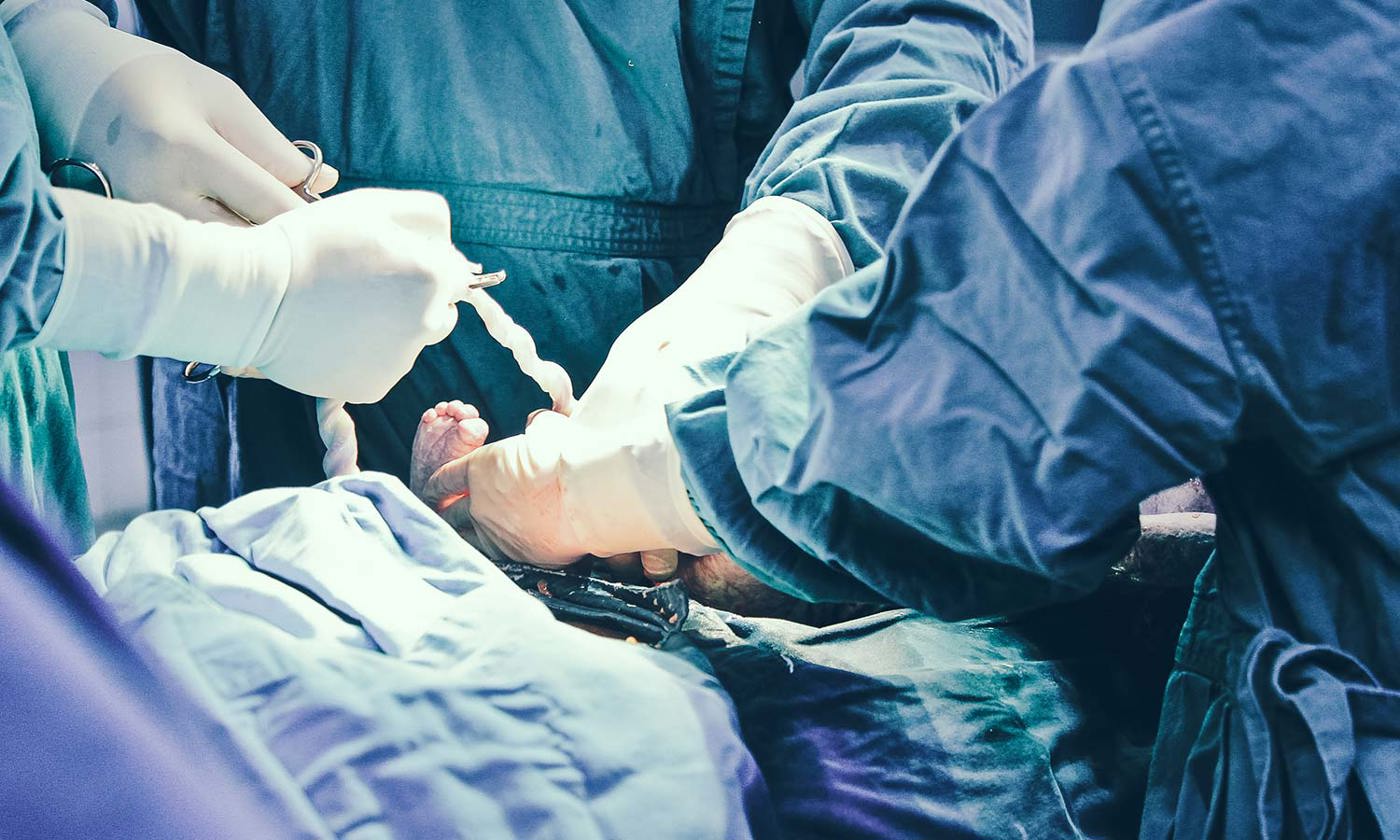
A caesarean section1 , or C-section, is an operation to deliver your baby through a cut made in your abdomen (tummy) and uterus (womb).
The cut is usually made across your tummy, just below your bikini line.
A caesarean is a major operation that carries a number of risks, so it's usually only done if it's the safest option for you and your baby.
Although the majority of Australian women have vaginal births (i.e. vaginal births including vaginal breech, forceps and vacuum), there appears to be a trend away from normal birth.
Australia has high rates of births by caesarean section (30.9% of births in 2007) compared with the OECD average of 25.7% of births. This rate is increasing in both the public and private sectors, but continues to be substantially higher in the private sector.
Why caesareans are carried out
A caesarean may be recommended as a planned (elective) procedure or done in an emergency if it's thought a vaginal birth is too risky. They're usually performed after the 38th week of pregnancy.
A caesarean may be carried out because:
- your baby is in the breech position (feet first) and your doctor has been unable to turn them by applying gentle pressure to your tummy, or you would prefer they didn't try this
- you have a low-lying placenta (placenta praevia)
- you have pregnancy-related high blood pressure (pre-eclampsia)
- you have certain infections, such as a first genital herpes infection occurring late in pregnancy or untreated HIV
- your baby isn't getting enough oxygen and nutrients – sometimes this may mean the baby needs to be delivered immediately
- your labour isn't progressing or there's excessive vaginal bleeding
If there's time to plan the procedure, your midwife or doctor will discuss the benefits and risks of a caesarean compared with a vaginal birth.
Asking for a caesarean
Some women choose to have a caesarean for non-medical reasons. If you ask your midwife or doctor for a caesarean when there aren't medical reasons, they will explain the overall benefits and risks of a caesarean compared with a vaginal birth.
If you're anxious about giving birth, you should be offered the chance to discuss your anxiety with a healthcare professional who can offer support during your pregnancy and labour.
If after discussion and support you still feel that a vaginal birth isn't an acceptable option, you're entitled to have a planned caesarean.
What happens during a caesarean
Most caesareans are carried out under spinal or epidural anaesthetic. This mean you'll be awake, but the lower part of your body is numbed so you won't feel any pain.
During the procedure:
- a screen is placed across your body so you can't see what's being done – the doctors and nurses will let you know what's happening
- a cut about 10-20cm long will usually be made across your lower tummy and womb so your baby can be delivered
- you may feel some tugging and pulling during the procedure
- you and you birth partner will be able to see and hold your baby as soon as they've been delivered
The whole operation normally takes about 40-50 minutes.
Occasionally a general anaesthetic, where you're asleep, may be used, particularly if the baby needs to be delivered more quickly.
Recovering from a caesarean
Recovering from a caesarean usually takes longer than recovering from a vaginal delivery.
The average stay in hospital after a caesarean is around three or four days. You may be able to go home sooner than this if both you and your baby are well.
While in hospital:
- you'll be given painkillers to reduce any discomfort
- you'll have regular close contact with your baby and can start breastfeeding
- you'll be encouraged to get out of bed and move around as soon as possible
- you can eat and drink as soon as you feel hungry or thirsty
- a thin, flexible tube called a catheter will remain in your bladder for at least 12 hours
- your wound will be covered with a dressing for at least 24 hours
When you're well enough to go home, you'll need to arrange for someone to give you a lift as you won't be able to drive for a few weeks.
When you go home, you'll need to take things easy at first. You may need to avoid some activities such as driving for six weeks or so.
The wound in your tummy will eventually form a scar. This may be red and obvious at first, but it should fade with time and will often be hidden in your pubic hair.
Risks of a caesarean
A caesarean is generally a very safe procedure, but like any type of surgery it carries a certain amount of risk.
It's important to be aware of the possible complications, particularly if you're considering having a caesarean for non-medical reasons.
Possible complications include:
- infection of the wound or womb lining
- blood clots
- excessive bleeding
- damage to nearby areas, such as the bladder or the tubes that connect the kidneys and bladder (ureter)
- temporary breathing difficulties in your baby
- accidentally cutting your baby when your womb is opened
Future pregnancies after a caesarean
If you have a baby by caesarean, it doesn't necessarily mean that any babies you have in the future will also have to be delivered this way.
Most women who have had a caesarean section can safely have a vaginal delivery for their next baby, known as vaginal birth after caesarean (VBAC).
However, you may need some extra monitoring during labour just to make sure everything is progressing well.
Some women may be advised to have another caesarean if they have another baby. This depends on whether a caesarean is still the safest option for them and their baby.
Although uncommon, having a caesarean can increase the risk of certain problems in future pregnancies, including:
- the scar in your womb opening up
- the placenta being abnormally attached to the wall of the womb, leading to difficulties delivering the placenta
- stillbirth
1 Contains public sector information licensed under the Open Government Licence v3.0.



